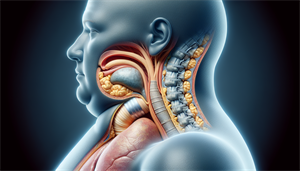
Have you ever tried sleeping with a mask connected to a machine? For many individuals suffering from sleep apnea, this nightly routine is all too familiar. Continuous Positive Airway Pressure (CPAP) therapy, the most common treatment for obstructive sleep apnea, requires users to wear a mask over their nose and/or mouth, hooked up to a device that delivers pressurized air to keep their airways open while they sleep.
But what if you need a different solution? How to sleep with sleep apnea without CPAP?
This blog post delves into alternatives to CPAP therapy for managing sleep apnea, including lifestyle modifications, oral device therapy, positional therapy, surgical interventions, and advanced therapies.
If you’re looking for a more comfortable, convenient, and personalized treatment for sleep apnea, you might find your answer here.
Key Takeaways
-
CPAP suppression therapy is the standard treatment for obstructive sleep apnea (OSA), but alternatives include positional therapy, oral appliance therapy, and surgical interventions for those who cannot tolerate CPAP.
-
Lifestyle changes such as weight management and optimizing sleeping positions are significant non-medical approaches that can improve or mitigate symptoms of sleep apnea.
-
A personalized treatment plan is crucial in the management of sleep apnea, considering individual needs and preferences to optimize outcomes and enhance treatment compliance.
Understanding Sleep Apnea and Non-CPAP Solutions

Severe obstructive sleep apnea, a common sleep disorder, is characterized by:
-
Recurrent partial or complete obstruction of the upper airway during sleep
-
Disrupted sleep
-
Daytime fatigue
-
Serious health complications if left untreated
The conventional treatment for this condition is the Continuous Positive Airway Pressure (CPAP) machine, which delivers a constant flow of air to keep the airway open during sleep.
However, not all patients can tolerate CPAP therapy, and some may look for alternatives. These may include:
-
Positional therapy
-
Oral device therapy
-
Surgery
-
Alternative PAP machines such as CPAP alternative devices
Before exploring alternatives to CPAP therapy, it’s advised to consult with a healthcare provider to guarantee the safety and effectiveness of the chosen treatment.
Defining Obstructive Sleep Apnea
Obstructive sleep apnea is primarily due to conditions that obstruct airflow through the upper airways during sleep. These include relaxed muscles in the head and neck, excess weight and obesity, and certain anatomical features. Age, sex, and underlying medical conditions such as heart failure, high blood pressure, and type 2 diabetes can also contribute to this condition in obstructive sleep apnea patients.
Doctors diagnose obstructive sleep apnea using various tests like polysomnography, which monitors sleep patterns and breathing. They also consider symptoms and sleep history when determining how to treat obstructive sleep apnea for the apt treatment of sleep apnea. In the process of treating obstructive sleep apnea, doctors aim to alleviate symptoms and improve overall health.
If left untreated, obstructive sleep apnea can lead to serious health complications, including cardiovascular issues, strokes, heart attacks, hypertension, type 2 diabetes, and more.
The Quest for CPAP Alternatives
Despite the effectiveness of CPAP therapy in managing sleep apnea, some individuals may seek alternatives due to factors such as comfort and convenience. For instance, one alternative is BiPAP, which provides two pressure settings and is more suitable for patients with complex respiratory conditions.
Oral appliance therapy is another alternative that uses devices worn during sleep to improve breathing. These appliances work by repositioning the lower jaw and tongue to keep the airway open. Expiratory Positive Airway Pressure (EPAP) devices and oral pressure therapy are other alternatives that can aid in managing sleep apnea symptoms.
Lifestyle Adjustments to Mitigate Sleep Apnea Symptoms

Although medical treatments can effectively reduce sleep apnea symptoms, making lifestyle adjustments also plays a significant role in managing this disorder. Effective weight management, for instance, can lead to improvements in sleep apnea symptoms and potentially even a cure, as excess weight contributes to the obstruction of the upper airways during sleep.
Another straightforward and impactful lifestyle adjustment is the optimization of sleeping positions. Side sleeping can help keep the airway from collapsing, a condition more probable when a person lies flat on their back. Abstaining from alcohol can also aid in alleviating sleep apnea symptoms, as alcohol has the potential to relax the throat muscles, exacerbating airway obstruction during sleep.
Weight Management Strategies
Research has shown that weight loss can reduce the severity of sleep apnea. This highlights the potential benefits of weight management for sleep apnea patients. Maintaining a moderate weight can result in symptom improvement, as obesity increases pressure on the upper airways, causing them to collapse during sleep.
Dietary modifications can also contribute to weight management and the improvement of sleep apnea symptoms. Here are some recommendations:
-
Increase the intake of fruits and vegetables
-
Choose foods rich in omega-3 fatty acids
-
Restrict the intake of alcohol, sugary beverages, dairy products, and high-fat foods
These changes can help alleviate sleep apnea symptoms by managing weight and improving sleep quality.
Specific exercises, such as tongue stretches, tongue push-ups, and yogic breathing, can also be beneficial in strengthening the throat muscles and reducing symptoms.
Optimizing Sleeping Positions
Sleeping on one’s side is generally considered more favorable for reducing sleep apnea symptoms compared to lying on the back. Avoiding the supine position can help decrease the number and severity of obstructive episodes, with side-sleeping, particularly on the left side, being more beneficial in reducing apnea.
To optimize side-sleeping, it is advisable to:
-
Adopt a mostly straight back while sleeping on the side
-
Research suggests that sleeping on the right side can be especially beneficial
-
Some individuals may experience symptom improvement by elevating the head while sleeping on their back.
Oral Device Therapy: A Viable CPAP Alternative

Oral device therapy offers a less intrusive alternative to CPAP machines for some individuals with mild to moderate sleep apnea. Comprising mandibular advancement devices (MADs) and tongue-retaining devices (TRDs), these devices operate by either advancing the lower jaw or retaining the tongue to maintain an open airway during sleep.
Though MADs are highly beneficial for people with mild obstructive sleep apnea or those who mainly experience OSA while sleeping on their backs, consulting with a healthcare professional before choosing these devices is vital. A dentist, in coordination with the healthcare professional, typically oversees the fitting and adjustments to mitigate any potential jaw complications or exacerbation of sleep apnea resulting from an ill-fitting device.
Mandibular Advancement Devices (MADs)
Mandibular advancement devices (MADs) are a therapeutic approach for obstructive sleep apnea and snoring. They work by advancing the lower jaw forward during sleep, effectively widening the airway and preventing its closure, thus addressing the symptoms of sleep apnea and snoring.
Despite their benefits, the efficacy rates for MADs in treating sleep apnea are below 40%, suggesting they may not be universally effective for all individuals with sleep apnea. Following the procedure, the recovery period typically spans from 2 to 4 weeks, with potential variations based on the individual and the scope of the surgical procedure.
Tongue Retaining Devices (TRDs)
Tongue retaining devices function by maintaining the tongue in a forward position while sleeping, thereby preventing its potential obstruction of the airway. They have demonstrated statistical effectiveness as an alternative therapy option for obstructive sleep apnea, resulting in an average reduction of 53% in apnea occurrences among users.
However, individuals using tongue retaining devices may encounter difficulties complying with their use, which can be attributed to discomfort or inconvenience.
Positional Therapy to Combat Sleep Apnea

Positional therapy is designed to promote side-sleeping position to prevent the relaxation of throat muscles and tongue, which can obstruct the airway and result in sleep apnea events. Wearable devices, like MORFEA and NightBalance, are designed to notify users when they are sleeping on their back, encouraging them to maintain a side-sleeping position throughout the night. This can potentially decrease the frequency of sleep apnea incidents.
Specialized pillows for sleep apnea include:
-
Wedge pillows that elevate the head
-
CPAP pillows that accommodate CPAP masks and reduce airway pressure
-
Side sleeper pillows that ensure proper spinal alignment
Selecting the appropriate pillow can significantly enhance sleep quality for individuals with sleep apnea.
Wearable Devices for Positional Therapy
Wearable devices for positional therapy utilize sensors to identify the user’s sleeping position. Upon detecting a supine position, the device either emits vibrations or alerts to prompt the user to transition to a lateral or side-sleeping position, which can aid in improving airflow and alleviating symptoms of sleep apnea.
Despite their benefits, several drawbacks of using wearable devices for positional therapy include:
-
Potential risk of data loss or analysis errors due to vulnerable wireless communication channels
-
Negative user experience
-
Limited device compatibility with different body types or sleep behaviors
-
Possibility of inaccurate readings
Specialized Pillows for Sleep Apnea
Specialized pillows for sleep apnea function by:
-
Facilitating correct alignment of the head, neck, and airway during sleep
-
Offering support and alleviating pressure on the airway
-
Aiding in the prevention of collapse and obstruction commonly experienced by individuals with sleep apnea
These pillows are specifically engineered to address the unique needs of sleep apnea sufferers.
Through the maintenance of a more open airway, these pillows can contribute to improved breathing and a reduction in the frequency and severity of apnea events during sleep.
Exploring Surgical Interventions
When other options fail to provide relief, some individuals with sleep apnea may consider surgical interventions. UPPP and hypoglossal nerve stimulation are among the surgical interventions that may be considered for the treatment of sleep apnea. It is important to note that while surgery can often decrease the severity of sleep apnea, it typically does not lead to a complete resolution of the condition. Following surgery, some individuals may still require the use of a CPAP machine to manage symptoms.
Surgery for sleep apnea carries potential risks such as:
-
Throat pain
-
Difficulty swallowing
-
Surgical complications
-
Other possible side effects
Hence, it’s imperative to seek advice from a healthcare provider before choosing surgical interventions.
UPPP and Soft Palate Surgery
UPPP surgery, also known as uvulopalatopharyngoplasty, and soft palate surgery are surgical interventions utilized to address obstructive sleep apnea. These procedures involve the removal and repositioning of tissue in the airway, with the goal of reducing the likelihood of airway collapse during sleep.
Despite their benefits, the efficacy rates for the treatment of sleep apnea with UPPP and soft palate surgery are below 40% and approximately 31.3%, respectively. These figures suggest that while some patients may benefit from the procedures, they may not be universally effective for all individuals with sleep apnea.
Hypoglossal Nerve Stimulation
Hypoglossal nerve stimulation entails the surgical implantation of a device in the upper chest, delivering electrical stimulation to the hypoglossal nerve to influence breathing. This process involves:
-
Detecting inspiratory effort during sleep
-
Triggering upper airway muscles to sustain airflow and avert airway collapse
-
Enhancing maximum inspiratory airflow
-
Reducing the critical closing pressure (Pcrit)
Although the procedure can be beneficial, it is important to note that hypoglossal nerve stimulation carries potential adverse effects such as:
-
tongue and lip weakness
-
infection
-
hematoma
-
pain
-
tongue abrasion
-
device malfunction
-
neuropraxia
-
sore tongue
-
swallowing difficulties
-
temporary tongue weakness and soreness.
Advanced Therapies Beyond CPAP
For individuals with sleep apnea who cannot tolerate or do not respond well to CPAP therapy, advanced therapies like bilevel positive airway pressure (BiPAP) and ASV machines provide alternative treatment options. BiPAP therapy and CPAP therapy both provide positive airway pressure to prevent airway collapse during sleep. However, BiPAP has two pressure settings, with a higher pressure for inhalation and a lower pressure for exhalation, making it more suitable for patients with complex respiratory conditions.
ASV therapy, also known as adaptive servo-ventilation therapy, is a non-invasive treatment primarily utilized for individuals with central sleep apnea (CSA). It involves:
-
Monitoring the patient’s breathing pattern
-
Automatically adjusting the pressure to stabilize the breathing
-
Correcting the irregular breathing patterns associated with CSA.
Despite their benefits, the potential adverse effects of BiPAP and ASV therapies may encompass:
-
Nasal, oral, or throat dryness
-
Nosebleeds
-
Bloating
-
General discomfort from the masks
-
Mask discomfort
-
Runny nose
-
Sinus pressure
-
Skin irritation
Consultation and Personalized Treatment Planning
In managing sleep apnea, a personalized treatment plan which takes into account the individual’s specific needs and characteristics is fundamental for a targeted and effective approach. Customizing the treatment plan allows healthcare providers to optimize outcomes and enhance the overall management of sleep apnea.
Treatment approaches for sleep apnea are tailored to the severity of the condition, often beginning with CPAP as the primary intervention for moderate to severe cases. In instances of mild sleep apnea, alternative options such as oral appliances may be considered. The presence of concurrent health conditions also significantly influences treatment decisions, as it may be essential to address sleep apnea alongside other conditions like cardiovascular or metabolic issues. The patient’s overall health is carefully considered to ensure a comprehensive and appropriate treatment plan.
The Role of a Sleep Disorder Evaluation
A sleep disorder evaluation is crucial for diagnosing sleep apnea and determining the most appropriate treatment options for each individual. This typically involves a sleep study or polysomnography, which monitors brain activity, breathing, and other physical processes during sleep. This process can help identify episodes of sleep apnea and aid in diagnosing the disorder.
Sleep disorder assessments are typically carried out by sleep specialists and sleep technologists who have received training in administering tests such as polysomnography and interpreting the results to identify sleep disorders such as apnea.
Tailoring Treatments to Individual Needs
When developing a treatment plan for a person with sleep apnea, it’s vital to consider factors like the severity of the condition, symptoms and sleep history, along with the patient’s age, sex, body weight, and anatomical features. Treatment goals typically revolve around enhancing sleep quality, reducing daytime sleepiness, and addressing snoring. Interventions may involve lifestyle adjustments like weight loss, exercise, avoiding alcohol and sedating medications, and modifying sleep positions.
Patient comfort and preference significantly influence the selection of treatment options for sleep apnea. Patients are more likely to comply with treatments that they find comfortable and convenient. For example, some patients may prefer oral appliances over CPAP therapy due to factors such as ease of use, portability, and quiet operation. It is essential to consider patient preferences as adherence to treatment is crucial for effectiveness.
Furthermore, incorporating patient feedback and goals is also vital in determining the most suitable treatment.
Summary
In conclusion, sleep apnea is a common sleep disorder that requires careful management to prevent serious health complications. While CPAP therapy is the most common treatment, it may not be suitable for everyone. Fortunately, there are many alternatives available, from lifestyle adjustments and oral device therapies to surgical interventions and advanced therapies beyond CPAP. Always consult with a healthcare provider to determine the most appropriate treatment options tailored to your specific needs and circumstances.
Frequently Asked Questions
Can you treat sleep apnea without a CPAP?
In conclusion, for mild sleep apnea, you can try lifestyle changes and fitted mouthpieces as non-CPAP options, but for moderate to severe sleep apnea, these alternatives are rarely successful.
How can I sleep if I don't have a CPAP machine?
You can manage sleep apnea without a CPAP machine by considering alternatives like oral appliances, bilevel positive airway pressure (BiPAP) machines, nasal valve therapy, lifestyle changes, or surgery. It's important to consult a healthcare professional to determine the most suitable treatment for your individual needs.
What is the best sleeping position for sleep apnea?
The best sleeping position for sleep apnea is on your side with your back mostly straight. This position can reduce apnea severity and snoring, as well as help maintain proper spine alignment.
Related health topics?
Some related health topics include the top 10 most common health issues. This can provide a useful overview of prevalent health concerns.
How effective are Mandibular Advancement Devices (MADs) in treating sleep apnea?
Mandibular Advancement Devices (MADs) are effective for some individuals with sleep apnea, but their efficacy rates in treating sleep apnea are below 40%, indicating that they may not work for everyone.