Are you feeling excessively tired during the day despite getting a full night’s sleep? Or perhaps your partner has expressed concerns about your abnormal breathing patterns while sleeping. If so, these could be indicators of a sleep disorder known as Central Sleep Apnea (CSA).
But what is central sleep apnea? CSA is not merely a disruption in your sleep cycle, but a signal that your body’s normal breathing mechanism is compromised during sleep.
While the symptoms may sound intimidating, understanding CSA, its causes, symptoms, and management options can empower you to seek help and restore your quality of life.
Key Takeaways
-
Central Sleep Apnea (CSA) is characterized by pauses in breathing due to the brain’s failure to signal the muscles that control breathing, affecting less than 1% of the population, mainly middle-aged/elderly individuals, and is associated with serious complications like cardiovascular issues.
-
The understanding of CSA’s physiology points to disrupted ventilation feedback loops and variations in PaCO2 levels as contributing factors, distinguishing it from Obstructive Sleep Apnea, which is due to physical blockages rather than signaling issues.
-
Management of CSA includes identifying symptoms (such as excessive daytime sleepiness, abnormal breathing during sleep), assessing for associated medical conditions (like heart failure or stroke), and exploring treatments like PAP therapies and lifestyle adjustments.
Unveiling Central Sleep Apnea
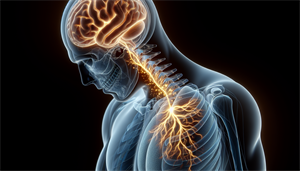
CSA is a sleep disorder characterized by the brain’s inability to send proper signals to the muscles responsible for breathing. This lapse in the communication system results in intermittent pauses in breathing during sleep, leading to fragmented sleep and daytime fatigue. While CSA affects less than 1% of the general population, it primarily impacts:
-
middle-aged or elderly individuals
-
exhibits a notable male predominance
-
it’s also infrequent in premenopausal women, potentially attributable to a lower apneic threshold of PaCO2 in women.
The complications of CSA go beyond disrupted sleep and excessive daytime sleepiness. It encompasses severe fatigue, irritability, difficulty in concentrating, and cardiovascular issues, severely impacting the quality of life of the affected individual. Therefore, if you are experiencing symptoms such as excessive daytime drowsiness, restless or poor quality sleep, or if a bed partner has reported abnormal breathing during sleep, it is advisable to seek medical advice. This is especially important for individuals with underlying conditions like congestive heart failure, as CSA can exacerbate their condition.
So, what causes CSA? Factors such as heart failure, stroke, or renal failure play a significant role in the onset of CSA. Individuals affected by these conditions typically exhibit a lower resting PaCO2 than normal, which may contribute to the breathing irregularities characteristic of CSA.
The Physiology Behind Central Sleep Apnea
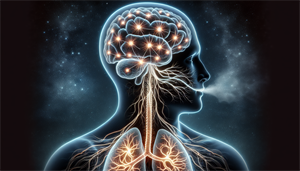
A proper understanding of CSA requires an exploration of its underlying physiology. CSA occurs when ventilation feedback loops are disrupted, leading to the brain’s failure in signaling the respiratory muscles and causing apneic episodes during sleep. This disruption is often attributed to increased sensitivity, or a high loop gain, within the system, resulting in abnormal breathing patterns.
Two types of phenomena constitute the pathophysiology of CSA: ventilatory instability and depression of brainstem respiratory centers or chemoreceptors. These phenomena can disrupt the regulation of breathing, leading to CSA syndromes. So, the issue lies not in the muscles that control breathing, but in the signals that regulate them.
So, how does PaCO2 contribute to the development of CSA? Variations in PaCO2 levels can trigger primary CSA by causing either hyperventilation leading to hypocapnia or general hypoventilation. These disruptions in PaCO2 levels directly affect the body’s capacity to sustain a consistent breathing rhythm during sleep, contributing to the onset of CSA.
Distinguishing Between Sleep Apnea Types
CSA and Obstructive Sleep Apnea (OSA) are two types of sleep disordered breathing. While both involve interruptions in breathing during sleep, the causes differ. In CSA, the brain fails to transmit appropriate signals to the respiratory muscles, resulting in pauses in breathing. Central sleep apnea occurs more frequently in individuals with certain medical conditions, such as heart failure or stroke. Understanding central sleep apnea syndromes can help in providing better treatment options for those affected.
The symptoms of CSA encompass:
-
Sudden awakenings accompanied by breathlessness
-
Insomnia
-
Excessive daytime drowsiness
-
Impaired concentration
-
Mood alterations
These symptoms may be more pronounced when compared to other types of sleep apnea, such as complex sleep apnea. For instance, individuals with severe central sleep apnea may encounter pronounced fatigue and difficulty concentrating, which may be more severe when contrasted with symptoms of other types of sleep apnea.
There is also a subtype of CSA known as primary CSA, which occurs independently without a distinct or identifiable cause. This suggests that CSA can manifest even without the presence of an underlying medical condition or the use of certain medications.
Recognizing the Symptoms of Central Sleep Apnea
The journey towards getting treatment for CSA begins with identifying its symptoms. The symptoms include snoring, excessive daytime sleepiness, and abnormal breathing patterns during sleep. These symptoms can often go unnoticed or be mistaken for other sleep disorders, making CSA a challenging condition to diagnose.
However, CSA does not just affect your sleep. It spills over into your daily life, resulting in insomnia, night awakenings, extreme fatigue, daytime drowsiness, irritability, morning headaches, and changes in mood such as depression or anxiety. These effects can impact your daytime functioning, leading to disrupted sleep, reduced energy, difficulty focusing, memory problems, and waking up feeling unrefreshed.
As such, if you or a loved one exhibit any of these symptoms, it is imperative to seek medical advice. Early detection and treatment can help manage CSA effectively and reduce the risk of potential complications.
The Root Causes of Central Sleep Apnea
CSA can be triggered by various factors, including medical conditions, drug use, and exposure to high altitudes. While these factors may seem unrelated, they all interfere with the body’s ability to regulate breathing during sleep, leading to the development of CSA.
A deep comprehension of these root causes is of paramount importance for the early detection, suitable treatment, and prevention of CSA. Therefore, let’s delve into these factors in more detail in the following subsections.
Medical Conditions Linked to CSA
Numerous medical conditions are associated with the onset of CSA. These include:
-
End-stage kidney disease
-
Stroke
-
Heart failure
-
Atrial fibrillation
-
Diabetes mellitus
-
Hypothyroidism
-
Parkinson’s disease
-
Multiple system atrophy
These medical conditions can disrupt the body’s normal breathing mechanism, making individuals with these conditions more susceptible to CSA.
For instance, CSA is present in around 10% of individuals who have experienced a stroke. A stroke can damage the part of the brain that controls breathing, leading to CSA. Similarly, the prevalence of CSA in patients with heart failure ranges from 25-40%, as heart failure can lead to fluid build-up in the lungs, causing difficulties in breathing and leading to CSA.
Hence, if you are diagnosed with any of these medical conditions, it’s imperative to understand the potential risk of developing CSA and have a discussion about it with your healthcare provider.
Drug-Induced Central Sleep Apnea
Certain drugs can contribute to CSA by inducing central nervous system depression, respiratory muscle dysfunction, or myopathy. Specifically, opioids and benzodiazepines can lead to irregular or halted breathing during sleep, thereby elevating the risk of CSA.
Opioids disrupt respiratory rhythm generation and ventilatory chemoreflexes, and suppress hypoglossal motoneuron and genioglossal muscle activity, leading to CSA. Similarly, central nervous system depressants like benzodiazepines diminish the function of dilator muscles, particularly during sleep, which can result in airway collapse and interruptions in breathing.
If you are on any of these medications, it’s critical to have a conversation with your healthcare provider about the possible risks of CSA. They may be able to adjust your medication regimen or monitor you for signs of CSA.
High Altitude and Its Effects on Breathing
High altitude can also lead to CSA. The reduction in oxygen levels at high altitudes can disturb the regular breathing patterns during sleep, leading to instances of paused or shallow breathing, which in turn causes episodes of CSA.
The physiological basis for high altitude periodic breathing, a form of CSA caused by high altitude exposure, is thought to be instability in the central respiratory drive induced by hypoxia. This instability can lead to periodic breathing and the development of central apneas during sleep.
Moreover, elevated altitudes can lead to reduced oxygen saturation levels in the body due to diminished atmospheric pressure, affecting the capacity of hemoglobin to bind with and transport oxygen throughout the body. Thus, if high altitude travel is a frequent part of your routine, it’s necessary to understand the potential risk of developing CSA.
Diagnosing Central Sleep Apnea

Diagnosing CSA is a multi-step process that involves evaluating the patient’s symptoms, medical history, and a physical examination. If CSA is suspected, an overnight sleep study is typically conducted to confirm the diagnosis.
An overnight sleep study is a diagnostic procedure that measures a person’s physiological functions during sleep. It is typically conducted in a specialized sleep laboratory, which may be located in a hospital or a designated sleep center. The study monitors various aspects of sleep, including breathing patterns, heart rate, and brain activity, providing a comprehensive assessment of the individual’s sleep health.
The process of diagnosing CSA also involves reviewing the patient’s sleep history, overnight monitoring, and potentially referring the patient to a sleep specialist. Hence, if you or a loved one are suspected to have CSA, it is critical to promptly seek medical attention.
Treatment Strategies for Central Sleep Apnea

Treatment for CSA typically involves addressing the underlying causes, improving the symptoms, and enhancing the quality of sleep. The most common treatment options include Positive Airway Pressure (PAP) therapies and alternative treatments, such as adaptive servo-ventilation, bilevel positive airway pressure, and the Remede System implant.
While these treatments can effectively treat CSA, their success varies among individuals, and some treatments may be more effective for certain types of CSA than others. Let’s further explore these treatment options in the subsections below.
Positive Airway Pressure Therapies
Positive Airway Pressure (PAP) therapies are essential in the treatment of CSA. PAP therapy delivers positive expiratory airway pressure (EPAP) and inspiratory pressure support (IPAP) to enhance ventilation and mitigate airway collapse during sleep.
Continuous Positive Airway Pressure (CPAP) therapy addresses CSA by utilizing a mask to administer a continuous flow of air pressure, thereby maintaining the openness of the airway during sleep and averting interruptions in breathing. Bi-level Positive Airway Pressure (BiPAP) therapy delivers two different levels of air pressure, with a higher pressure during inhalation and a lower pressure during exhalation. This approach is beneficial for individuals with CSA as it helps to regulate their breathing pattern, leading to improved oxygen levels and assistance with breathing challenges during sleep.
It should be noted, however, that some individuals may develop central sleep apnea, known as treatment emergent central sleep, during the course of CPAP therapy. This condition involves a mixture of obstructive and central sleep apneas during CPAP treatment. In some cases, this condition may improve with consistent use of the CPAP device.
Alternative and Emerging Treatments
Apart from PAP therapies, there are alternative and emerging treatments available for CSA. These include adaptive servo-ventilation (ASV), bilevel positive airway pressure (BiPAP), and the Remede System implant.
ASV is a non-invasive ventilatory treatment that utilizes a device to deliver servo-controlled pressure support, promoting regular breathing patterns in individuals with CSA. BiPAP delivers air into the lungs at two different pressure settings, with a higher pressure during inhalation and a lower pressure during exhalation. The Remede System functions as an implantable device that monitors the patient’s respiratory signals and stimulates the diaphragm to facilitate normal breathing.
These treatments offer hope for individuals with CSA, providing a range of options that can be tailored to meet their specific needs and conditions. It should be highlighted that the effectiveness of these treatments may vary from one individual to another, making it necessary to discuss these options with a healthcare provider to devise the best suited treatment plan.
Living with Central Sleep Apnea

Living with CSA can be challenging, but it’s certainly manageable. The key lies in effectively managing symptoms, adhering to treatment plans, and making lifestyle adjustments to improve sleep quality and overall health.
CSA can be managed daily by:
-
Controlling underlying conditions
-
Using breathing assistance devices like PAP machines
-
Maintaining an optimal weight
-
Steering clear of known triggers
-
Sticking to a consistent sleep schedule
-
Making lifestyle modifications such as changing sleep position and maintaining proper hydration
Regular guidance from healthcare professionals also plays a crucial role in managing CSA.
Lifestyle changes that can aid in the prevention of CSA include:
-
Weight reduction
-
Cessation of alcohol and smoking
-
Adherence to a balanced diet
-
Regular physical exercise
These changes not only help manage the symptoms of CSA but also contribute to a healthier and more fulfilling life.
Prevention and Risk Factor Mitigation
Preventing CSA and reducing risk factors involves managing underlying medical conditions, steering clear of certain medications, and exercising caution while ascending to high altitudes.
Addressing underlying medical conditions such as heart failure, stroke, kidney failure, atrial fibrillation, Parkinson’s disease, hypothyroidism, and multiple system atrophy can help mitigate the risk of developing CSA. It is also recommended to refrain from using medications such as long-acting benzodiazepines, narcotics, opioids, and certain sedative-hypnotic agents as these medications can impair the brain’s capacity to effectively regulate the breathing muscles.
Lifestyle modifications can also decrease the likelihood of CSA. These include:
-
Weight loss
-
Regular exercise
-
Cessation of smoking and alcohol consumption
-
Avoidance of specific medications
-
Adherence to a consistent sleep routine
Additionally, if you frequently travel to high altitudes, it’s crucial to ascend gradually, maintain proper hydration, and consider the use of medications like acetazolamide to adapt to the high altitude environment.
Summary
In conclusion, CSA is a complex sleep disorder characterized by the brain’s inability to send proper signals to the muscles responsible for breathing. While it primarily affects middle-aged or elderly individuals, it can occur in anyone, particularly those with certain medical conditions or lifestyle factors.
Diagnosis involves a multi-step process, and treatment options range from PAP therapies to alternative and emerging treatments. Living with CSA involves managing symptoms, adhering to treatment plans, and making lifestyle adjustments.
Prevention and risk factor mitigation strategies include addressing underlying medical conditions, avoiding certain medications, and being cautious when ascending to high altitudes. While living with CSA can be challenging, with the right knowledge and management strategies, individuals with CSA can lead healthy, fulfilling lives.
Frequently Asked Questions
What is the difference between central sleep apnea and sleep apnea?
The main difference between central sleep apnea and sleep apnea is that in obstructive sleep apnea, the airway is blocked, causing snoring and sleep fragmentation, while in central sleep apnea, the issue is with the brain signaling the muscles that control breathing. Central sleep apnea is less common than obstructive sleep apnea.
What is the most common cause of central sleep apnea?
The most common cause of central sleep apnea is opioids such as methadone, while it can also be associated with congestive heart failure or stroke. It can also occur shortly after ascending to high altitudes.
How is central apnea treated?
Central sleep apnea can be treated with positive airway pressure (PAP) therapy, supplemental oxygen, medication, or an implantable nerve stimulation device. The choice of treatment depends on the cause of the condition and the individual's breathing patterns and needs.
Can central sleep apnea get better?
Central sleep apnea can improve in some cases with chronic CPAP therapy, but it may persist despite regular CPAP treatment, and other treatments such as therapy for heart failure or reduction of opioid medicines may also help.
Symptoms of sleep apnea?
Common symptoms of sleep apnea include: [Add specific symptoms from previous answers here]. If you experience any of these, it's important to consult a healthcare professional for a proper diagnosis and treatment.


