Sleep Apnea, a commonly underestimated sleep disorder, presents a unique challenge to both its sufferers and medical professionals. It’s like a stealthy night prowler, often going unnoticed and undiagnosed, yet leaving a trail of exhaustion, frustration, and health issues.
But what if you could spot this prowler before it wreaks havoc on your health? Understanding “what are the warning signs of sleep apnea”, health consequences, risk factors, and treatment options for sleep apnea could be your first step towards reclaiming restful nights and energetic days.
Key Takeaways
-
Sleep apnea is characterized by symptoms such as loud snoring, disrupted breathing during sleep, excessive daytime fatigue, and morning headaches, which can severely impact one’s quality of sleep and overall health.
-
Untreated sleep apnea can lead to serious health consequences including cardiovascular issues, hypertension, metabolic disorders like type 2 diabetes, and mental health problems such as depression and cognitive impairment.
-
Treatments for sleep apnea include the use of CPAP machines, which are considered the gold standard, as well as alternative therapies, surgical interventions, and lifestyle changes such as weight loss and improving sleep hygiene.
Unveiling the Symptoms of Sleep Apnea

Understanding sleep apnea’s common indicators is a crucial step in combating it. Sleep apnea often manifests in:
-
Loud snoring
-
Disrupted breathing during sleep
-
Gasping for air and disrupting sleep rhythm
-
Excessive tiredness during the day, even after a full night’s rest
-
Morning headaches, a silent warning sign that sleep patterns have been disrupted due to interrupted breathing
These are just a few warning signs, or tell-tale symptoms of sleep apnea.
However, a deeper understanding of these symptoms is necessary.
Interrupted Breathing: More Than Just Snoring
While snoring often becomes the brunt of jokes, it can signal a serious issue. Sleep apnea is not just about loud snoring; it involves a complex interplay of disrupted breathing patterns. Obstructive sleep apnea, one of the two primary classifications of the condition, can lead to sleep apnea snores, which are caused by:
-
a narrowing or complete closure of the airway due to the relaxation of throat muscles
-
lower oxygen levels in the blood
-
brief awakenings to reopen the airway, leading to disrupted sleep
This leads to sleep interruption, depriving you of the deep, restorative sleep stages necessary for high-quality rest.
Daytime Fatigue Despite a Full Night's Rest
A common misconception about sleep apnea is that if you sleep through the night, you’re safe. The reality is, even after a full night’s sleep, individuals with sleep apnea often experience:
-
Daytime fatigue
-
Severe daytime drowsiness
-
Fatigue
-
Irritability
These symptoms result from repeated pauses in breathing, known as apneas, which prevent individuals from reaching deeper, restorative stages of sleep. These awakenings affect daily functioning and performance.
Therefore, if you’re experiencing excessive daytime sleepiness despite a full night’s rest, it could indicate a battle with sleep apnea.
Waking Up with a Start: Gasping and Choking at Night
Imagine being jolted awake in the middle of the night, gasping or choking for air. This can be a reality for individuals suffering from sleep apnea, including central sleep apnea. The obstruction or collapse of the upper airway during sleep leads to reduced oxygen and increased carbon dioxide levels in the body, prompting the brain to awaken the individual to resume normal breathing.
The brain is typically responsible for maintaining steady breathing during sleep, but in cases of sleep apnea, airway collapse can result in breathing interruptions and symptoms such as gasping or choking. Such episodes can be evaluated using the Apnea-Hypopnea Index (AHI), which tallies the occurrences of apneas and hypopneas per hour during sleep. A higher AHI signifies a more critical instance of sleep apnea, frequently associated with increased occurrences of gasping or choking episodes.
The Health Consequences of Ignoring Sleep Apnea

Neglecting sleep apnea doesn’t make it vanish; instead, it paves the way for various health issues. Untreated sleep apnea can result in:
-
Cardiovascular complications including coronary heart disease, high blood pressure, stroke, heart failure, and cardiac arrhythmia
-
Metabolic disorders such as type 2 diabetes
-
Hypertension
-
Mental health issues
Even the use of certain medicines and undergoing major surgery can become complicated due to the increased risk of complications following sedation.
Sleep Apnea and Hypertension: A Dangerous Duo
Sleep apnea and hypertension make for a dangerous duo. These two conditions often exist side-by-side, exacerbating each other and increasing the risk of heart disease and stroke. The connection between sleep apnea and hypertension is fortified by:
-
Acute and chronic increases in sympathetic activation
-
Elevated blood pressure
-
Potentially causing structural changes in the aortic wall that worsen hypertension.
For instance, about 70-83% of individuals with sleep apnea also have hypertension, showing a significant overlap between the two conditions. On a positive note, treating sleep apnea, particularly through the use of CPAP therapy, can help reduce blood pressure levels and significantly enhance the control of hypertension.
The Link Between Sleep Apnea and Metabolic Disorders
The battle with sleep apnea extends into the realm of metabolic disorders. Sleep apnea is correlated with an elevated risk of metabolic disorders, such as type 2 diabetes and liver problems, due to its impact on glucose levels and insulin resistance. It’s quite alarming that over half of those with type 2 diabetes also have sleep apnea.
Moreover, sleep apnea occurs and there is a documented correlation between it and liver conditions such as nonalcoholic fatty liver disease (NAFLD), which is defined by the accumulation of excess fat in the liver.
Mental Fog and Mood Instability
The effects of sleep apnea aren’t confined to physical health; they seep into mental health, too. Sleep apnea can induce mood disorders like depression and anxiety and is also linked to increased irritability and mood fluctuations. Chronic fatigue from sleep apnea can lead to daytime sleepiness, cognitive impairment, difficulty concentrating, irritability, and mood instability.
Effectively managing sleep apnea can mitigate these symptoms, enhancing overall mood and well-being.
Risk Factors That Elevate Your Chances of Sleep Apnea
Certain factors can increase your susceptibility to sleep apnea. From physical traits like obesity and neck circumference to lifestyle choices, these factors determine your risk of developing this sleep disorder. Being overweight or obese is a significant risk factor, and an enlarged neck circumference can exacerbate the likelihood of the condition due to potential airway blockage from excess fat deposits.
Conversely, lifestyle choices like smoking and alcohol consumption can increase your risk of developing sleep apnea.
Weight and Neck Circumference: Physical Indicators
Obesity and a larger neck circumference are physical indicators that can contribute to sleep apnea. Excessive body weight, especially a high body mass index (BMI), is regarded as a prominent risk factor for obstructive sleep apnea. Excess fat deposits in the upper respiratory tract can narrow the airway, potentially inducing sleep apnea episodes.
Also, larger necks, measuring more than 16 or 17 inches in circumference, are associated with narrower airways, which can lead to breathing difficulties during sleep, potentially inducing sleep apnea episodes.
Lifestyle Choices: Alcohol, Smoking, and Sleeping Positions
The way we live our lives can significantly impact our health, including our sleep health. Alcohol consumption can exacerbate sleep apnea by intensifying drops in blood oxygen levels and disrupting breathing patterns during sleep. Smoking leads to persistent inflammation in the upper airway, which can exacerbate sleep apnea symptoms.
Identifying and understanding these lifestyle risks, as well as considering one’s family history, is a step towards managing sleep apnea and enhancing overall health.
Diagnosing Sleep Apnea: What to Expect from a Sleep Study
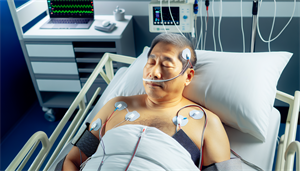
Once you recognize the symptoms and risk factors of sleep apnea, the next step is getting a proper diagnosis. A sleep study, also known as polysomnography, is typically used to diagnose sleep apnea. The diagnostic process involves the placement of surface electrodes on the face and scalp to record electrical signals, as well as the attachment of sensors to the chest, limbs, and finger to monitor breathing, heart rate, and sleep patterns.
This procedure aids in identifying problems like frequent breathing interruptions, a telltale sign of sleep apnea.
Treatment Pathways: From CPAP to Lifestyle Changes
After diagnosis, the path to managing sleep apnea encompasses a variety of treatment options, including:
-
Continuous Positive Airway Pressure (CPAP) machines
-
Alternative therapies
-
Surgical interventions
-
Lifestyle modifications
The choice of treatment depends on the severity of the condition and individual preference.
CPAP: The Gold Standard in Sleep Apnea Treatment

CPAP machines typically serve as the primary treatment method for sleep apnea. They provide continuous positive airway pressure, keeping the airway open during sleep and facilitating easier breathing. CPAP therapy is recognized as highly effective in treating sleep apnea, improving neurobehavioral and cardiovascular consequences of the condition, and enhancing overall quality of life for individuals with sleep apnea.
Beyond CPAP: Alternative Therapies and Surgical Options
For those who find it difficult to tolerate CPAP treatment, alternative therapies and surgical options exist. Oral appliances like Mandibular Advancement Devices (MADs) and Tongue Stabilizing Devices (TSD) can help by repositioning the lower jaw, improving airflow, and maintaining an open airway during sleep.
Upper airway stimulation therapy, which delivers mild stimulation to help the throat muscles relax during sleep, can also aid in maintaining an open airway.
Lifestyle Interventions: Weight Loss and Sleep Hygiene
Lifestyle interventions can also play a significant role in managing sleep apnea. Weight loss, in particular, can significantly impact sleep apnea symptoms. In some instances, a mere 10% reduction in body weight can have a remarkable effect.
Furthermore, adopting good sleep hygiene can alleviate sleep apnea symptoms and address contributors like obesity and improper sleep positioning.
Summary
Understanding sleep apnea is the first step towards reclaiming a healthy sleep cycle. Recognizing the symptoms, knowing the risk factors, and availing the right treatment can significantly improve your quality of life. With the knowledge you’ve gained from this blog post, you’re now equipped to take control of your sleep health. Remember, sleep is not a luxury, it’s a necessity. So, take a step today for a better, healthier sleep tomorrow.
Frequently Asked Questions
What is the most telling symptom of sleep apnea?
The most telling symptom of sleep apnea is loud snoring often punctuated by gasping or choking sounds, especially when it is reported by another person. Other symptoms include morning headaches, dry mouth upon awakening, and restless sleep with periods of wakefulness during the night.
What can be mistaken for sleep apnea?
Common conditions that can be mistaken for sleep apnea include asthma, allergies, and chronic obstructive pulmonary disease (COPD). Be sure to consult a healthcare professional if you suspect sleep apnea.
How can I test myself for sleep apnea?
You can test yourself for sleep apnea with a home sleep apnea test, which is a portable breathing monitor that you wear overnight. It monitors your breathing and oxygen levels to detect pauses in breathing while you sleep.
What is the first stage of sleep apnea?
The first stage of sleep apnea is benign snoring. Benign snoring is often harmless, but it can indicate a potential development of sleep apnea in the future.
What are the health risks associated with untreated sleep apnea?
Untreated sleep apnea can lead to serious health risks including cardiovascular complications, metabolic disorders, and mental health issues. It's important to seek treatment to avoid these potential consequences.


