Are you experiencing jaw pain, facial discomfort, or headaches? Have you ever wondered if these symptoms could be related to a condition called temporomandibular joint disorder (TMJ)?
In this article, we will delve into the world of TMJ disorders, exploring the anatomy, causes, symptoms, diagnosis, and treatment options available. We will also discuss how you can manage TMJ disorders at home and when to seek professional help.
By the end, you will have a thorough understanding of TMJ disorders and feel empowered to take control of your jaw health.
Key Takeaways
-
Gaining an understanding of Temporomandibular Joint Disorder requires knowledge of jaw anatomy and function, along with the various causes and treatments that may be associated with it.
-
Identifying the causes involves analyzing potential physical/emotional stressors, poor posture, oral health issues & injuries to the jaw.
-
Seeking professional help from a TMJ specialist is essential for accurate diagnosis & appropriate treatment. Regular dental checkups are key prevention strategies.
Understanding Temporomandibular Joint Disorder
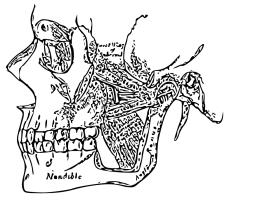
Temporomandibular joint disorders, or temporomandibular joint TMJ disorders, refer to a group of health conditions affecting the jaw and the muscles controlling it, collectively known as temporomandibular disorders TMD.
The temporomandibular joint is a hinge joint that provides the connection between the lower jaw and temporal bones of the skull. It allows for movement such as eating, talking and yawning. TMJ disorders can be caused by various factors, such as:
-
strain on the jaw joints and muscles
-
bruxism (teeth grinding)
-
injury
-
arthritis
-
displacement of the jaw joint disks.
Treatment for TMJ disorders depends on factors such as symptoms, age, overall health, and the severity of the condition. Gaining a thorough understanding of TMJ disorders necessitates a look at jaw anatomy and function, along with the various forms of TMJ disorders that may arise.
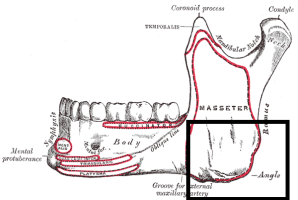
Jaw Anatomy and Function
The comprehension of TMJ disorders heavily relies on the knowledge of jaw anatomy and function. The temporomandibular joints (TMJ) enable the mandible (lower jaw) to move in multiple directions, including:
-
Upwards
-
Downwards
-
Sidewards
-
Forwards
-
Backwards
This allows us to perform activities such as chewing, speaking, yawning, and swallowing.
Jaw muscles, joints, and nerves work together to enable seamless jaw movements. When these components are affected by injury, inflammation, or other issues, TMJ disorders can arise, causing pain and discomfort.
Types of TMJ Disorders
There are various types of TMJ disorders, each with different causes and symptoms. Some of the most common types include:
-
Jaw muscle disorder
-
Temporomandibular joint dysfunction (TMD)
-
Degenerative joint disease (DJD)
-
Other structural changes to the temporomandibular joint
Jaw muscle disorder occurs when the muscles controlling the jaw become tight, weak, or uncoordinated, leading to pain and clicking or popping of the jaw. TMD is characterized by inflammation or irritation of the temporomandibular joint, resulting in pain and difficulty opening and closing the mouth, as well as jaw locking. DJD involves the deterioration of cartilage within the temporomandibular joint, causing pain and limited jaw movement.
Other structural changes may include misalignment of the jaw, dislocation of the jaw, and fractures of the jaw, all of which can result in pain and difficulty opening and closing the mouth.
Proper treatment is contingent on accurately identifying the specific type of TMJ disorder.
Identifying the Causes
Potential causes of TMJ disorders include physical and emotional stress, poor posture, and oral health issues. Physical and emotional stress may contribute to the development of TMJ disorders by causing muscle tension, teeth clenching, or grinding. Poor posture and oral health issues, such as misaligned teeth or jaw injuries, can also lead to TMJ disorders.
Other known causes of TMJ disorders include:
-
Injuries to the jaw, joint, or muscles of the head and neck
-
Heavy blows or whiplash
-
Trigger points (contracted muscles in the jaw, head, and neck that refer pain to other areas, causing headaches, earaches, or toothaches)
A more profound comprehension of how physical and emotional stress, poor posture, and oral health contribute to TMJ disorders is crucial for understanding prevention and treatment methods.
Physical and Emotional Stress
Physical and emotional stress can contribute to TMJ disorders by inducing muscle tension and teeth clenching or grinding. Stress can cause the muscles in the jaw to tense up, resulting in pain and discomfort. Additionally, stress can lead to jaw clenching or grinding, which can further exacerbate pain and discomfort.
Implementing stress management techniques, such as deep breathing exercises, meditation, or yoga, can help reduce tension and alleviate TMJ symptoms.
Poor Posture and Oral Health
Poor posture and oral health issues play a significant role in TMJ disorders. Maintaining a forward head posture while using a computer for prolonged periods can cause strain on facial and neck muscles, leading to TMJ symptoms.
Poor posture, such as hunching or slouching, can put strain on bones and joints, including the temporomandibular joint, leading to:
-
Misalignment
-
Popping
-
Locking
-
Cramping
-
Pain in the jaw joints
Additionally, misaligned teeth and jaw injuries can contribute to TMJ disorders. Addressing posture and oral health issues can help reduce the risk of developing TMJ disorders.
Recognizing the Symptoms
Proper diagnosis and treatment of TMJ disorders hinge on the ability to recognize the TMD symptoms. Common symptoms include:
-
Aching of the jaw
-
Facial discomfort
-
Headaches
-
Ear pain
-
Clicking or popping sounds in the jaw
-
Difficulty opening or closing the mouth
If you experience recurrent jaw pain, facial pain, headaches, or other TMJ symptoms, it’s essential to seek medical assistance. It’s important to note that tooth decay, sinus problems, arthritis, and gum disease can also manifest with similar symptoms, so a thorough examination by a healthcare provider is necessary to confirm a TMJ disorder diagnosis.
Examining specific symptoms like jaw pain, discomfort, facial pain, and headaches will aid in understanding their correlation with TMJ disorders.
Jaw Pain and Discomfort
Jaw pain and discomfort are common symptoms of TMJ disorders, often accompanied by difficulty opening and closing the mouth. Jaw pain can be attributed to:
-
Physical and emotional stress
-
Poor posture
-
Oral health issues
-
Grinding or clenching the teeth
-
Misalignment of the jaw
-
Arthritis
Indications of jaw pain include:
-
Difficulty opening and closing the mouth
-
Pain or tenderness in the jaw
-
Headaches
-
Neck pain
-
Clicking or grating sounds in the jaw joint
Should persistent jaw pain be experienced, consulting a healthcare provider for appropriate diagnosis and treatment becomes vital.
Facial Pain and Headaches
Facial pain and headaches can also be indicative of TMJ disorders, as they may result from muscle tension and joint inflammation. These symptoms, along with jaw pain and discomfort, can significantly impact your quality of life and may warrant further investigation by a healthcare provider.
It’s important to remember that physical and emotional stress, poor posture, and oral health issues can also contribute to facial pain and headaches, so a proper examination is necessary to determine the root cause of these symptoms.
Diagnosis Process
The diagnosis process for TMJ disorders primarily involves a thorough history and physical examination. There is no standard test available to diagnose TMD, so symptoms and jaw movement are typically assessed to ascertain the presence of TMD. In some cases, imaging tests, such as X-rays or jaw bone scans, may be employed to supplement the diagnosis.
A comprehensive evaluation and accurate diagnosis necessitate consultations with healthcare providers, dentists, and ear, nose, and throat doctors. Exploring the specialists’ consultation process and the imaging techniques used for diagnosing TMJ disorders will be insightful.
Consultation with Specialists
Consultations with healthcare providers, dentists, and ear, nose, and throat doctors are essential for a thorough examination and accurate diagnosis of TMJ disorders. These specialists have the expertise to:
-
Assess your symptoms
-
Perform a physical examination
-
Recommend further testing, such as imaging tests, if necessary
-
Provide suitable treatment options tailored to your individual condition
To prepare for your appointment, it’s important to compile all pertinent medical information, including past medical history, current medications, and any recent imaging tests.
Imaging Techniques
Imaging techniques, such as X-rays and MRI scans, can help identify the underlying causes of TMJ symptoms and guide treatment plans. X-rays provide images of the bones and joints, while MRI scans generate detailed images of the soft tissues, such as muscles, tendons, and ligaments. These imaging tests can help determine if there are any structural abnormalities or inflammation in the temporomandibular joint that may be contributing to your symptoms.
In some cases, imaging tests may not be necessary, and your healthcare provider may rely on physical examination findings and your medical history to diagnose your TMJ disorder.
Non-Surgical Treatment Options
Non-surgical treatment options for TMJ disorders include medications and pain relievers, physical therapy, and relaxation techniques. These treatments aim to alleviate symptoms, control pain, and improve jaw function.
Depending on the severity of your condition, your healthcare provider may recommend a combination of these treatment options to provide the best possible outcome. It’s important to remember that each person’s experience with TMJ disorders is unique, and what works for one person may not necessarily work for another. Working closely with your healthcare provider to devise a treatment plan that suits you is of paramount importance.
Examining medications and pain relievers, alongside physical therapy and relaxation techniques, will shed light on management methods for TMJ disorders.
Medications and Pain Relievers
Medications and pain relievers, both over-the-counter and prescription, can help alleviate TMJ symptoms and inflammation. Over-the-counter nonsteroidal anti-inflammatory drugs (NSAIDs), such as ibuprofen and naproxen, as well as acetaminophen, can provide relief from pain and inflammation. Prescription medications for TMJ disorders may include muscle relaxants, tricyclic antidepressants, and corticosteroids.
It’s important to consult with your healthcare provider before starting any medication to ensure it’s safe and appropriate for your specific condition. They can also advise on the proper dosage and potential side effects.
Physical Therapy and Relaxation Techniques
Physical therapy and relaxation techniques can also help improve TMJ symptoms and overall jaw function.
Physical therapy techniques may include:
-
Exercises to enhance jaw mobility, posture, and strength
-
Manual therapy to minimize pain and inflammation
-
Relaxation techniques to alleviate stress and tension.
Stress management exercises, such as deep breathing, progressive muscle relaxation, and mindfulness activities like yoga and meditation, can help reduce muscle tension in the jaw and prevent teeth clenching or grinding. Working with a physical therapist or healthcare provider experienced in treating TMJ disorders can ensure you receive the most effective treatment for your specific needs.
Surgical and Invasive Procedures
Surgical and invasive procedures for TMJ disorders include arthroscopy, arthrocentesis, and open-joint surgery. These procedures are typically considered when non-surgical treatment options have not provided sufficient relief.
However, surgery for TMJ disorders should be viewed as a last resort, as it can sometimes worsen symptoms and cause additional complications. Discussion on potential risks, benefits, and alternatives with your healthcare provider becomes imperative before considering surgery or any invasive procedure.
A detailed examination of Botox injections and considerations for surgery in TMJ disorders will be beneficial.
Botox Injections
Botox injections have been shown to play a role in treating TMJ disorders by temporarily relaxing the muscles in the jaw, reducing pain, and relieving symptoms such as headaches. Studies have indicated that Botox may provide long-term relief by decreasing the intensity, frequency, and duration of TMJ symptoms. However, it’s important to note that the use of Botox for TMJ disorders is still considered experimental.
Discussing the potential benefits and risks of Botox injections with your healthcare provider can help determine if this treatment option is suitable for your specific condition.
Surgery Considerations
Surgery for TMJ disorders, such as arthrocentesis or jaw repair/replacement, can provide relief for certain cases when more conservative treatments have failed. However, surgery carries risks and potential complications, such as infection, nerve damage, and worsening of symptoms.
It’s essential to carefully consider these risks and potential complications, as well as discuss alternative treatment options, with your healthcare provider before opting for surgery.
Remember, surgery should be considered as a last resort for TMJ disorders.
Managing TMJ Disorders at Home
Managing TMJ disorders at home involves making lifestyle changes, practicing stress management, and maintaining a healthy diet. By taking proactive steps to address the causes and symptoms of TMJ disorders, you can help prevent the condition from worsening and significantly improve your quality of life. In some cases, making these changes may be enough to alleviate symptoms without the need for more invasive treatments.
Exploring lifestyle modifications, stress management techniques, and dietary recommendations can be instrumental in managing TMJ disorders at home.
Lifestyle Changes
Lifestyle changes, such as improving posture and avoiding teeth clenching or grinding, can help prevent TMJ disorders from worsening. Good posture can reduce strain on the jaw muscles and joints, while refraining from teeth clenching and grinding can reduce strain on the jaw muscles and joints.
By making these simple changes, you can help reduce the risk of developing TMJ disorders and improve your overall jaw health.
Stress Management and Diet
Stress management techniques and a balanced diet can contribute to overall jaw health and reduce the risk of TMJ disorders.
Some techniques to consider include:
-
Deep breathing exercises
-
Progressive muscle relaxation
-
Yoga
-
Meditation
Implementing these relaxation exercises and mindfulness activities can help alleviate stress and tension in the jaw.
A nutritious diet consisting of ample amounts of fruits and vegetables, lean proteins, and whole grains can help manage TMJ disorders by reducing inflammation and supplying the body with essential nutrients. Additionally, avoiding processed foods and sugary snacks can help reduce the likelihood of developing TMJ disorders.
Prevention Strategies
Prevention strategies for TMJ disorders include regular dental checkups and avoiding teeth clenching and grinding. By taking preventative measures, you can help reduce the risk of developing TMJ disorders and maintain your overall oral health. Preventative strategies can also help identify potential issues early on, allowing for more effective treatment and management.
Examining the significance of regular dental checkups for maintaining upper and lower teeth health, and the avoidance of teeth clenching and grinding as preventative measures against TMJ disorders will be insightful.
Regular Dental Checkups
Regular dental checkups can help identify potential issues early on and prevent the development of TMJ disorders. Dentists are able to detect early signs of TMJ disorders during routine examinations and can provide suitable treatment or preventive measures.
Additionally, maintaining good oral hygiene through regular brushing and flossing can help prevent gum disease, tooth decay, and other oral health issues that may contribute to TMJ disorders. By prioritizing regular dental checkups and maintaining good oral health, you can help prevent TMJ disorders and ensure a healthier jaw.
Avoiding Teeth Clenching and Grinding
Avoiding teeth clenching and grinding is an essential prevention strategy for TMJ disorders. Teeth clenching and grinding can cause excessive strain on the jaw muscles and joints, leading to the development or worsening of TMJ disorders.
Practicing relaxation techniques, such as deep breathing exercises and progressive muscle relaxation, can help reduce stress and tension in the jaw, preventing teeth clenching and grinding. By consciously avoiding these harmful habits, you can help reduce the risk of developing TMJ disorders.
Seeking Professional Help
Seeking professional help for TMJ disorders involves finding a TMJ specialist and preparing for your appointment. A TMJ specialist, such as a dentist or healthcare provider with experience in treating TMJ disorders, can provide an accurate diagnosis and recommend the most appropriate treatment options for your specific condition. It’s essential to consult with a specialist if you’re experiencing persistent jaw pain, facial pain, headaches, or other symptoms that impede your quality of life.
Discussing the process of locating a TMJ specialist and preparing for your appointment is crucial to secure the best possible care for your TMJ disorder.
Finding a TMJ Specialist
Finding a TMJ specialist is crucial for proper diagnosis and treatment of your TMJ disorder. Specialists such as dentists, physical therapists, and other healthcare professionals with experience in treating TMJ disorders can provide the expertise needed for an accurate diagnosis and tailored treatment plan. You can obtain a referral from your primary care physician or search online for a TMJ specialist in your area.
Once you’ve found a specialist, it’s important to prepare for your appointment by compiling all pertinent medical information, including past medical history, current medications, and any recent imaging tests.
Preparing for Your Appointment
Preparing for your appointment with a TMJ specialist ensures you receive the best possible care for your condition. When scheduling your appointment, be sure to provide information regarding your symptoms, medical history, and any medications you’re currently taking.
During your appointment, you can expect to discuss your symptoms, undergo a physical examination and diagnostic tests, and receive a diagnosis and treatment recommendation. By being well-prepared and proactive in addressing your TMJ disorder, you can work closely with your specialist to find the most effective treatment options for you.
Summary
In this article, we have explored the complex world of temporomandibular joint disorders, providing a comprehensive understanding of the anatomy, causes, symptoms, diagnosis, and treatment options available. By recognizing the symptoms, seeking professional help, and implementing prevention strategies and home management techniques, you can take control of your jaw health and improve your quality of life.
Remember, early intervention and a proactive approach to managing TMJ disorders are crucial in preventing further complications and ensuring the best possible outcome.
Frequently Asked Questions
How do you fix temporomandibular disorder?
To fix temporomandibular disorder, treatment may include resting the TMJ, taking medication or pain relievers, and practicing relaxation techniques, making behavior changes, receiving physical therapy, wearing an orthopedic appliance or mouthguard, and posture training.
What happens if TMJ is left untreated?
Left untreated, TMJ can cause facial swelling, muscle spasms and uneven development, and in severe cases may necessitate surgery to correct permanent damage to the jaw bones.
Does temporomandibular disorder go away?
TMDs can be short-term and resolve on their own, but in some cases they can become chronic or co-occur with other medical conditions.
How serious is temporomandibular disorder?
Temporomandibular disorder (TMD) can cause persistent discomfort, tension in the jaw area, inflammation of the joints and even damage to your teeth if left untreated. In some cases, it can lead to severe pain, restricting patients' diet and leading to malnutrition, and possibly even long-term jaw damage if corrective measures are not taken.
How can I relieve my TMJ?
To relieve your TMJ, try improving your posture, reducing stress, getting a good night's sleep, using a hot or cold compress, exercising your jaw, avoiding bad habits and certain activities and foods, and maintaining the resting position of your jaw.
References
- Temporomandibular Disorders: Current Concepts and Controversies in Diagnosis and Management. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC8000442/
- Temporomandibular Joint Disorders: A Review of Etiology, Clinical Management, and Tissue Engineering Strategies. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4349514/
- Temporomandibular Joint Disorders (TMD). https://www.joms.org/article/S0278-2391(21)00663-7/fulltext


