Many are curious if their nighttime snoring could be the culprit behind a dry cough. Directly put, can snoring cause dry cough? The answer is yes, as snoring can indeed cause dry cough by irritating the upper airway.
This irritant leads to a dry cough as a common symptom and may be tied to conditions such as Upper Airway Cough Syndrome (UACS). In this discussion, we’ll delve into how snoring influences dry coughs and how managing one could ease the other.
Key Takeaways
-
Snoring may cause physical trauma and inflammation to the upper airway, leading to chronic cough especially with conditions like Obstructive Sleep Apnea (OSA).
-
Gastroesophageal Reflux Disease (GERD) during sleep, or nocturnal reflux, can significantly contribute to coughing due to upper esophageal irritation.
-
Management of allergic rhinitis, including avoiding allergens and using medication like antihistamines and nasal corticosteroids, can reduce cough symptoms related to post-nasal drip.
The Connection Between Snoring and Dry Cough

Far from being just an annoyance to those sharing your bed, snoring might indicate a deeper health concern. Snoring occurs when airflow through the mouth and nose is physically obstructed. This obstruction can be influenced by various factors, including nasal and sinus problems, being overweight, or simply the way you’re built. You might wonder how this connects to a dry cough?
It turns out, there’s a correlation between chronic cough and snoring due to irritation in the upper airway. This association can be related to conditions such as Upper Airway Cough Syndrome (UACS). Moreover, sleep apnea, specifically obstructive sleep apnea (OSA), is frequently observed in individuals with chronic cough.
OSA results in disrupted breathing during sleep, which may trigger or worsen a chronic cough. Furthermore, a cough may result from airway inflammation, which can be caused by various factors including environmental elements like air pollution and medical conditions such as obstructive sleep apnea syndrome (OSAS).
Upper Airway Irritation
Snoring isn’t merely a bothersome sound that fills the night. It has the potential to:
-
elevate upper airway resistance
-
induce weakening of muscle tone in the intercostal and pharyngeal muscles
-
cause physical trauma
-
cause peripheral nerve injuries.
Additionally, snoring may contribute to upper airway collapse and flow restriction, ultimately leading to sleep apnea in patients with obstructive sleep. This results in upper airway injury and inflammation, which in turn leads to throat irritation and a subsequent dry cough reflex.
The direct link between snoring and upper airway irritation therefore provides a clear explanation for why snorers often wake up with a dry cough. The physical trauma caused by chronic snoring leads to inflammation and irritation that the body responds to by triggering a cough reflex.
Sleep Apnea and Chronic Cough
Sleep apnea, a common reason for snoring, plays a role in chronic cough. It does so through numerous mechanisms such as:
-
Inflaming the airway
-
Causing repeated instances of airway blockage
-
Raising levels of inflammatory substances like interleukin-6, interferon-gamma, and interleukin-8
This can also be seen in chronic obstructive pulmonary disease (COPD).
Symptoms such as snoring, nocturnal cough, and unexplained chronic cough, particularly when traditional investigations and treatment trials are ineffective, can indicate the presence of sleep apnea in patients. In addition, it has been reported that the prevalence of OSA is notably high in patients with chronic cough. This highlights the potential connection between the two conditions..
Indeed, CPAP therapy has been documented to be effective for OSA-related cough. It plays a role in:
-
improving the underlying airway inflammation
-
addressing chronic nocturnal cough, especially in the supine position
-
potentially influencing cough sensitivity
Moreover, noticeable improvement in cough symptoms can be observed within one month of commencing CPAP therapy.
Disrupted Sleep Patterns
Beyond being a disruptive noise that interrupts your or your partner’s sleep, snoring signifies more. It’s a sign of disrupted sleep patterns that can exacerbate dry cough symptoms. This is because disrupted sleep patterns can induce physical discomfort, dryness in the throat and mouth, and postnasal drip, which can affect cough reflex sensitivity.
Indeed, disrupted sleep patterns resulting from snoring can worsen dry cough symptoms, potentially causing them to become more severe or enduring, and may contribute to idiopathic chronic cough. This essentially means that the cough has no identifiable cause despite thorough investigation.
As such, enhancing sleep patterns and minimizing snoring could play a role in lessening symptoms of a dry cough. This can be achieved by maintaining a healthy body mass index (BMI), which can help alleviate snoring and its associated symptoms.
Gastroesophageal Reflux Disease (GERD) and Cough
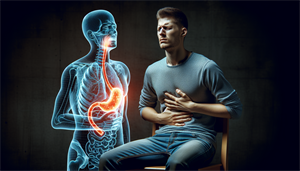
Gastroesophageal Reflux Disease (GERD) is yet another medical condition that could contribute to a persistent cough. GERD is characterized by the flow of stomach acid back into the esophagus, leading to irritation and various symptoms such as heartburn, wheezing, and a sore throat.
GERD can trigger a cough through a phenomenon known as nocturnal reflux. This is when, during sleep, the stomach contents flow back into the esophagus, causing irritation and leading to coughing. GERD may have a significant impact on sleep-disordered breathing (SDB) and its associated cough, as it is frequently cited as a leading cause of chronic cough within the context of SDB.
Chronic cough in non-smokers with normal chest radiographs and pulmonary functions can be caused by conditions such as GERD, cough-variant asthma (CVA), and upper airway cough syndrome (UACS). These can lead to persistent coughing despite no abnormalities being visible on chest X-rays and lung function tests. Therefore, it’s important to consider GERD as a possible underlying cause when dealing with a persistent cough.
Nocturnal Reflux
Nocturnal reflux, also referred to as nighttime acid reflux or gastroesophageal reflux disease (GERD) occurring during sleep, can result in a cough as the stomach contents flow back up into the esophagus. This reflux not only irritates the esophageal lining but also triggers coughing as a reflex response to alleviate the irritation.
Indications of nocturnal reflux encompass:
-
Heartburn
-
Chest pain
-
Chronic coughing
-
Wheezing
-
Difficulty in initiating sleep
Nocturnal reflux can result in snoring due to the potential damage caused by the upward flow of stomach acid to the esophageal lining, leading to inflammation and constriction of the airways.
Thus, managing nocturnal reflux can potentially help in reducing snoring and the associated dry cough. It’s crucial to remember that each individual is unique, and what works for one person might not work for another.
GERD Management
The management of GERD can aid in alleviating cough symptoms by addressing the underlying cause of the cough, which is frequently the reflux itself. Lifestyle modifications that can help manage GERD include:
-
Maintaining a healthy weight
-
Avoiding late meals
-
Refraining from lying down after eating
-
Elevating the head during sleep
These lifestyle changes can help alleviate cough symptoms associated with GERD.
Dietary changes should include:
-
Avoidance of common triggers such as chocolate, caffeine, onions, and carbonated drinks
-
Reducing the intake of fats and simple sugars
-
Increasing fiber intake
These changes can be beneficial for managing certain conditions.
Typical medications prescribed for the management of GERD include proton pump inhibitors (PPIs) such as omeprazole and esomeprazole, as well as histamine blockers. It’s important to consult with a healthcare provider to determine the most appropriate treatment plan for your condition.
Allergic Rhinitis and Cough
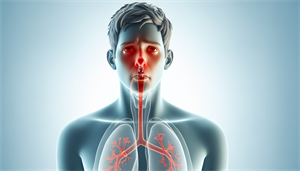
A cough can also be a result of another condition, allergic rhinitis. This happens through a mechanism called post-nasal drip, which occurs as a response to the inflammation and mucus production in the nasal passages.
Post-nasal drip refers to the accumulation of mucus in the posterior part of the throat. This surplus mucus can trickle down the throat, leading to irritation that initiates coughing as the body endeavors to expel the irritant.
The symptoms of a cough caused by allergic rhinitis can be managed through appropriate treatment of the allergic condition. This may involve the use of antihistamines, nasal corticosteroids, and the avoidance of known allergens to minimize inflammation and post-nasal drip.
Post-Nasal Drip
Post-nasal drip is a condition characterized by the accumulation of excess mucus in the throat or back of the nose, often associated with chronic rhinitis, such as allergic rhinitis. Typical triggers for post-nasal drip in individuals with allergic rhinitis include:
-
the condition itself
-
other types of rhinitis such as non-allergic rhinitis
-
sinusitis
-
the excessive use of nasal sprays
Post-nasal drip stemming from allergic rhinitis has the potential to induce coughing, as the surplus mucus descends the throat, prompting cough reflexes and irritation. Snoring worsens the cough associated with post-nasal drip by elevating intra-pharyngeal pressure, resulting in an open mouth posture and a posterior tongue base.
This heightened pressure increases the vibration of throat soft tissues, leading to snoring and potentially causing upper airway injury and inflammation, thereby exacerbating the cough.
Managing Allergic Rhinitis
Managing allergic rhinitis through medication can assist in reducing cough symptoms by addressing the underlying inflammation and irritation of the nasal passages. Some common medications used for the management of allergic rhinitis include:
-
OTC antihistamines
-
Expectorants
-
Decongestants
-
Nasal irrigation
-
Steam inhalation
-
Corticosteroid nasal sprays
These medications can help alleviate cough symptoms and provide relief from allergic rhinitis.
Individuals with allergic rhinitis can alleviate symptoms by refraining from exposure to allergens, cigarette smoke, and pets. Environmental changes play a crucial role in minimizing contact with irritants and allergens that can trigger or exacerbate the symptoms of allergic rhinitis, consequently reducing associated cough symptoms as well.
It’s important to remember that individual responses to treatments may vary, and what works for one person may not work for another. Therefore, it’s always better to consult a healthcare provider to find the most appropriate treatment plan.
Lifestyle Changes to Reduce Snoring and Dry Cough

Lifestyle alterations can have a substantial effect on reducing the intensity of snoring and dry cough. These include weight management, adjusting sleep position, and smoking cessation.
Managing weight can potentially lessen snoring by reducing the pressure on the neck and rib cage exerted by extra fat, thus enhancing the breathing pathways. A study demonstrated an 85 percent reduction in cough linked to sustained weight loss, suggesting a positive impact on reducing dry cough as well.
Adjusting sleep position to facilitate improved breathing can contribute to reducing snoring and cough symptoms by averting airway blockage and lessening the effects of postnasal drip.
Giving up smoking can assist in lowering airway irritation, improving lung function and corticosteroid responsiveness, as well as decreasing inflammation in the airway.
Weight Management
Obesity can lead to snoring as a result of neck fat compressing the upper airway, which in turn leads to snoring. Moreover, being overweight or obese can also lead to an excess of soft tissue in the mouth and throat, further increasing the likelihood of snoring.
Weight gain can impact our airways and lead to snoring through the presence of neck fat that compresses the upper airway and obstructs the flow of air. Additionally, the accumulation of pharyngeal fat can block the upper airway during sleep, contributing to snoring.
Weight loss has the potential to significantly decrease snoring, especially when complemented with other strategies like sleeping on one’s side and using a nasal decongestant. The maintenance of a healthy weight can contribute to the reduction of snoring and associated cough symptoms by alleviating the pressure on the upper airways and reducing the risk of conditions such as GERD, which can lead to a persistent cough.
Sleep Position
Modifying sleep position to facilitate improved breathing can contribute to reducing snoring and cough symptoms by averting airway blockage and lessening the effects of postnasal drip. The most effective sleep positions for reducing snoring and dry cough are sleeping on your side to prevent airway blockage and avoiding sleeping on your back, which can exacerbate conditions such as postnasal drip.
Elevating the head while sleeping is effective in reducing snoring and dry cough by maintaining open airways, enhancing breathing, and relieving post-nasal drip, which is a contributing factor to coughing. There are specific pillows and aids, such as anti-snore pillows, that come highly recommended. These pillows are designed to align the head and shoulders to keep airways open, and elevating the head with such a pillow can facilitate easier breathing and help control postnasal drip.
Smoking Cessation
Giving up smoking can assist in lowering airway irritation, improving lung function and corticosteroid responsiveness, as well as decreasing inflammation in the airway. Smoking leads to airway irritation as a result of inflammation from irritants present in cigarette smoke. This irritation prompts the body to cough as a means of clearing the airways.
Indeed, there is a known association between smoking and an increased likelihood of experiencing snoring and obstructive sleep apnea. The irritation caused by smoke from tobacco products can contribute to these conditions, and current smokers are at a higher risk of developing obstructive sleep apnoea compared to former or never-smokers.
Recommended methods for quitting smoking include:
-
Nicotine replacement therapy
-
Prescription medications
-
Behavioral counseling
-
Having a clear understanding of one’s personal motivation to quit.
When to Seek Medical Help
Even though lifestyle modifications can considerably relieve snoring and dry cough symptoms, it remains crucial to seek medical attention when warning signs appear or when symptoms persist despite these changes. Indicators suggesting the need for immediate medical intervention include:
-
Excessive daytime sleepiness
-
Loud snoring
-
Observed episodes of stopped breathing during sleep
-
Waking during the night and gasping or choking
Failing to address persistent snoring and dry cough can result in upper airway injury, inflammation, and obstructive sleep apnea (OSA).
Pulmonologists and otolaryngologists (ENT specialists) are the medical professionals most suited for addressing snoring and dry cough issues. It’s important to remember that each individual is unique, and what works for one person might not work for another. Therefore, it’s always better to consult a healthcare provider to find the most appropriate treatment plan.
Warning Signs
Symptoms such as difficulty breathing or chest pain, accompanied by other signs associated with snoring and dry cough, warrant immediate medical attention. Excessive daytime sleepiness, loud snoring, observed episodes of stopped breathing during sleep, waking during the night and gasping or choking are indications that prompt seeking medical attention without delay.
If an individual experiences chest pain or difficulty breathing, particularly after a prolonged period, and these symptoms are accompanied by indications of a heart attack, angina, or pulmonary embolism, it is advisable to seek immediate medical assistance.
Persistent cough and snoring can serve as indicators of serious underlying conditions such as obstructive sleep apnea, which entails upper airway injury and inflammation due to frequent episodes of interrupted breathing during sleep. Therefore, it’s crucial to pay attention to these warning signs and seek medical help when necessary.
Treatment Options
There are a variety of treatment options for snoring and dry cough, ranging from medication and CPAP therapy to surgery, all dependent on what’s causing the conditions. Typical medications prescribed for snoring and dry cough include benzonatate, guaifenesin, and dextromethorphan.
However, it’s important to note that based on three trials, it was found that antihistamines did not show significant effectiveness compared to a placebo in alleviating cough symptoms. This suggests that many over-the-counter cough medications may not provide substantial relief for treating dry cough associated with snoring.
Continuous Positive Airway Pressure (CPAP) therapy aids in the treatment of snoring and dry cough by maintaining positive airway pressure to prevent collapse and obstruction, thereby reducing the likelihood of snoring and associated dry cough.
Uvulopalatopharyngoplasty (UPPP) and soft-palate implants (Pillar procedure) are considered to be highly effective surgical options for addressing snoring related to sleep apnea.
Summary
To summarize, snoring and dry cough are common issues that individuals face, and they could be interlinked through various mechanisms such as upper airway irritation, sleep apnea, and disrupted sleep patterns. Conditions like GERD and allergic rhinitis can also contribute to a cough. Lifestyle changes such as weight management, sleep position adjustments, and smoking cessation can significantly alleviate these symptoms. However, it’s crucial to seek medical help when experiencing warning signs or when symptoms do not improve despite implementing these changes. Remember, the key is to listen to your body and seek medical advice when necessary.
Frequently Asked Questions
Why am I getting dry cough during sleep?
A dry cough during sleep can worsen due to factors like gravity, dry air, or increased airway sensitivity. It's important to understand these potential triggers and consider seeking medical advice if the cough persists.
What is the treatment for sleep apnea cough?
The most common treatment for sleep apnea cough is CPAP therapy, which stands for Continuous Positive Air Pressure therapy. It is the recommended option for moderate and severe OSA.
Can snoring cause a dry cough?
Yes, snoring can cause a dry cough due to upper airway irritation, sleep apnea, and disrupted sleep patterns. It is important to address snoring to alleviate these symptoms.
How does GERD lead to a cough?
GERD can lead to a cough due to nocturnal reflux, which causes stomach contents to irritate the esophagus during sleep, leading to coughing.
How can weight management reduce snoring and dry cough?
Weight management can reduce snoring by alleviating pressure on the neck and rib cage caused by excess fat, thereby improving breathing pathways. This, in turn, can also alleviate dry cough. Try incorporating weight management techniques to see if it helps improve your symptoms.